Giovanni Liguori is a staff writer for Brief Policy Perspectives and a first-year MPP student.
With the COVID-19 pandemic affecting every aspect of daily life and obligating lawmakers to address the public health crisis, one can’t help but think about other times in US history when such actions have been needed or considered before. Perhaps the most recent example of an unknown disease wreaking havoc on the world population is the Human Immunodeficiency Virus (HIV) epidemic. Over the past 40 years, this epidemic has had an incredible trajectory, going from being ignored almost entirely by the US government to a cure becoming one of the world’s most well-funded research endeavors. Additionally, much of the policy implemented to address HIV that helped effectively control the spread of the disease has influenced governments’ decisions for the COVID-19 pandemic.
In the early days of its discovery, the virus was originally thought to only inflict gay men and was colloquially termed “gay-related immune deficiency,” or GRID. This stemmed from the fact that, at first, the mysterious symptoms associated with HIV were primarily reported by homosexual men. By 1983, when the HIV virus was officially discovered and attributed as the cause of AIDS, 70% of the afflicted were gay or bisexual men. The Center for Disease Control (CDC) subsequently deemed homosexuals to be a high-risk group for AIDS. This mischaracterization of the illness being a “gay disease” cast irreparable damage onto the country’s already marginalized and fearful LGBTQ+ communities.
By 1986, cases of HIV had been found in practically every part of the world, from the US to China to Africa. While desperately researching and testing a cure, President Reagan established a commission on the disease in 1987. Human trials of a vaccine began that same year thanks to help from the Food and Drug Administration. Despite these steps forward, Congress took a notable step back; the Helms AIDS Amendment was passed, which withheld federal funding from “AIDS education, information, or prevention materials and activities that promote, encourage, and condone homosexual sexual activities.” The country also banned all foreign visitors who were diagnosed with AIDS from entering the country. The beginning responses to this epidemic were riddled with homophobia and discrimination.
Major breakthroughs in government action on the crisis began in the early 1990s. Congress passed the Ryan White CARE Act in 1990, which provided funding for HIV treatment and resources when insurers largely turned their backs on those infected with the disease. Later that year, they gained further protection from discrimination under the Americans with Disabilities Act (ADA). As President, Bill Clinton took a much more active approach to combating HIV and AIDS in comparison to his predecessors. Clinton appointed AIDS Czar Kristine Gebbie, established the Presidential Advisory Council on HIV/AIDS (PACHA), dramatically increased funding for a cure and therapy, and planned to have a vaccine within a decade. Prevention programs were also emphasized, aiming to educate the public on HIV’s signs and causes. By 1996, the Highly Active Anti-Retroviral Treatment (HAART) revolutionized the outlook and everyday life of those with the disease; the famed three-drug cocktail worked effectively to suppress the virus and protect the immune system of those infected with it from weakening severely and developing AIDS. Though not a cure, this therapy transformed HIV from an eventual death sentence to a livable condition.
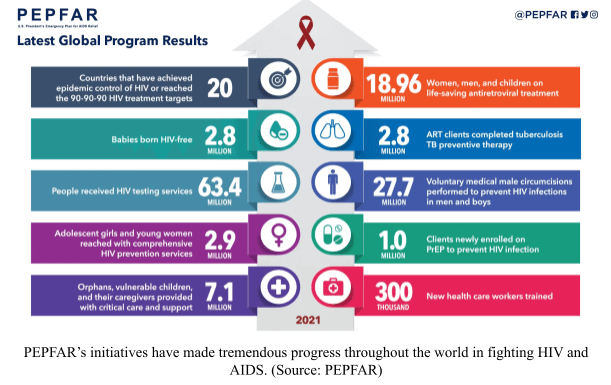
Now with the spread and fear of HIV less of an issue domestically, the country began shifting its focus to rooting out the disease internationally as well. Under George W. Bush, the U.S. President’s Emergency Plan for AIDS Relief (PEPFAR) was founded to raise money to fight HIV and AIDS abroad. Across almost 20 years and $85 billion from the federal government, the initiative has prevented nearly 20 million deaths from HIV through expanded access to testing, treatments, and prevention methods. Especially in developing regions where the virus is rampant such as Africa, these tools help those afflicted understand their HIV status and curtail further health deterioration or spread of the virus. The fund is still active today.
The National Institute of Health (NIH) also invests the most money in the world towards researching more effective treatment and eventually a cure for the disease. Domestically, President Obama further dismantled a troubling existing international issue in one of his first acts as president by allowing HIV-positive foreigners to enter the country. Obama shifted the narrative of prevention from conservatively-driven abstinence-only education to effective sex education. Under the Trump administration in 2019, the country launched the highly ambitious Ending the HIV Epidemic in the U.S. initiative, which seeks to reduce HIV infections by at least 90% by 2030. The plan includes needle exchange programs, treatments involving fewer pills or responsibility of the patient, and increased access to Pre-Exposure Prophylaxis (PrEP), which is highly effective in preventing HIV infection. Though there has been no vaccine yet approved to prevent or cure HIV, the groundbreaking success of COVID-19 mRNA vaccines has created new optimism for an HIV inoculation. HIV mRNA vaccines are currently in trial and have demonstrated encouraging results in producing immune responses in non-humans, according to the National Institute of Allergy and Infectious Diseases (NIAID). These promising outcomes could see an end for HIV on the horizon.
There have been several lessons learned from the HIV epidemic that informed the way the United States combatted the current COVID-19 pandemic. For starters, both diseases have shown that delayed action or inaction altogether has disastrous effects on the country as a whole. Nearly 40 years later, we are still searching for a cure that can root out HIV for good, which may be the case for COVID as well. However, without the billions of dollars invested in antiviral research, therapy, and experimentation stemming from HIV, we may not have been equipped with the tools to develop and utilize effective treatments for COVID. Furthermore, the COVID pandemic response has largely been about mitigation and harm reduction, focusing on reducing spread rather than eradication, the same course of action followed for HIV.
With the COVID-19 pandemic still unfolding, the United States can look back at the way it previously dealt with an unknown virus for precedent on how to deal with the current public health crisis. Over time, thanks to activism, investment, and scientific advances, treatment of the disease became widespread and those who are HIV positive people can live fully normal and healthy lives. The policy to address the HIV epidemic vastly shifted based on the political priorities of those in the White House and Congress. Future policy should focus on reducing all new infections by rooting out geographic and demographic inequalities in those most prone to infection. By employing an intersectional approach to address HIV, the United States could end the global HIV epidemic once and for all.
